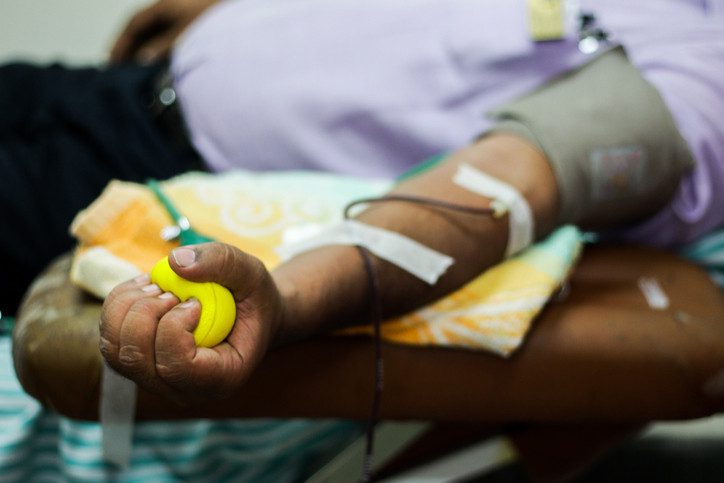
The blood supply in the US is critically low. Donations dropped off so dramatically during the COVID-19 pandemic that the American Red Cross has declared a national blood crisis. And since donated red blood cells only last about six weeks, supplies cannot be stockpiled in advance. A severe shortage could require difficult decisions about who should or shouldn’t receive a transfusion — decisions with life-or-death consequences.
So it makes sense to eliminate unnecessary restrictions on who can donate blood, right? And yet, one group of potential blood donors — men who have sex with men (MSM) — is not eligible to donate blood if they’ve been sexually active in the last three months, according to FDA guidelines.
Why single out men who have sex with men?
Such restrictions were first applied in the 1980s. HIV, the virus that causes AIDS, had not yet been discovered, but it had become clear that men who had sex with men were at particularly high risk for AIDS. Additionally, researchers learned that HIV could be transmitted through blood, including blood transfusions. The lifetime restriction on blood donations made by gay and bisexual men that quickly became policy was intended to help stop the spread of AIDS.
What’s the justification now?
More than 40 years later, the viral cause of AIDS is well established and detection tools have advanced.
- Highly accurate blood tests can detect HIV.
- Potential blood donors are asked about risk factors for HIV and other infections that can spread through a blood donation.
- Donated blood is routinely tested so that tainted blood is not transfused.
Yet not until 2015 was the lifetime ban on blood donation revised by the FDA to allow donation by MSM who reported being abstinent for a full year. When blood donations plummeted during the pandemic, restrictions were revised again. Currently, men who have sex with men can choose to donate blood as long as they attest to not having had sex with men for three months.
Why three months? The concern is that even with highly accurate testing, a recently acquired infection could be missed.
Vital steps to keep the blood supply safe
Of course it’s vitally important to keep the blood supply safe. No system is perfect, but the safety track record of transfused blood in the US is remarkably good: transfusion-related infections such as HIV and hepatitis are exceedingly rare. For HIV, the estimated risk of infection by transfusion is well under one in a million in this country.
Blood banks achieve this high safety standard through
- Questionnaires that seek to disqualify people whose donation could cause illness in the recipient. For example, potential blood donors are asked detailed questions about risk factors for infection and medicines they take. Of course, this relies on accurate and honest self-reporting.
- Testing donated blood: Regardless of answers to the screening questions, all donated blood is routinely tested for a number of transmissible infections, including
- hepatitis B and C
- HIV
- syphilis
- West Nile virus.
Not surprisingly, blood testing is much more reliable than self-reporting. The spectacularly accurate testing available now is far more effective than an honor system that asks potential donors about risk factors for having an infectious disease.
That’s one big reason behind increasing calls for changes in the blood donation policies that apply to MSM. Research underway now may help with policy decisions. The ADVANCE study (Assessing Donor Variability And New Concepts in Eligibility) is examining the impact of changing the screening questionnaire to ask gay and bisexual men about specific behaviors that raise infection risk, rather than requiring sexual abstinence for the previous three months. For example, having unprotected sex with multiple partners or being paid for sex are high-risk activities, regardless of one’s sex or sexual orientation.
The bottom line: Who can safely donate blood?
Currently, no compelling evidence shows that blood donation by men who have sex with men compromises the safety of our blood supply. Policies that require a period of abstinence for MSM may exclude many people at low risk for having an infection spread through blood, while allowing others at higher risk to donate.
Many countries focus on individual risk factors for infections that can be transmitted through a blood transfusion, not a person’s sex or sexual orientation. Britain, France, Israel, and other countries use such policies to keep their blood supplies safe. The American Medical Association, American Red Cross, and several US senators support similar policies for the US — an approach also backed by many experts in the field.
In my view, a change in blood donation policy is long overdue: all donor eligibility should be based on medically justified risk factors, and all potential donors should be screened the same way. And the sooner these restrictions are lifted, the better. A just, equitable, and medically sound blood donation policy is not only the right choice — it could allow donation of blood that saves your life.
Commenting has been closed for this post.
Source by www.health.harvard.edu